Cardiac Catheterization
Quick Facts
- Cardiac catheterization is a common procedure done to see how well your heart works.
- A cardiac catheterization can also be used to do procedures to open blocked arteries or valves.
- It is done in a hospital or clinic.
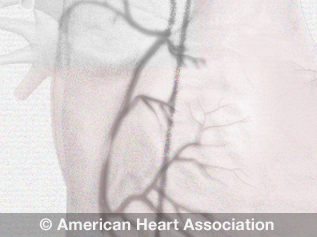
What is cardiac catheterization?
Cardiac catheterization (cardiac cath or heart cath) is a procedure to see how well your heart works. It is used to diagnose some heart problems. It is one of the most common heart procedures performed in the U.S.
View an illustration of cardiac catheterization(link opens in new window).
Why do people have cardiac catheterization?
A cardiac cath provides information on how well your heart works, identifies problems and allows for procedures, such as angioplasty and stenting, to open blocked arteries. During a cardiac cath your health care team may:
- Take X-rays using contrast dye to look for narrowed or blocked coronary arteries. This is called coronary angiography or percutaneous transluminal coronary arteriography.
- Perform a percutaneous coronary intervention (PCI), such as coronary angioplasty with stenting, to open narrowed or blocked segments of a coronary artery.
- Perform a valvuloplasty to widen a narrowed heart valve opening.
- Check the pressure in the four chambers of your heart.
- Take samples of blood to measure the oxygen content in the four chambers of your heart.
- Look for defects in the valves or chambers of your heart.
- Remove a small piece of heart tissue (biopsy) to examine under a microscope.
Watch an animation of an angiogram
What are the risks of cardiac catheterization?
Cardiac cath is usually very safe. Major complications are very rare. Some minor risks include:
- Bruises where the catheter was inserted (puncture site)
- Bleeding at the puncture site
- Reaction to the contrast dye
- Infection
- Side effects, such as nausea or vomiting, from the medications given to help you relax or sleep during the procedure
Some other risks include:
- Abnormal heart rhythm
- Blood clots
- Damage to a blood vessel or heart from the catheter
- Heart attack
- Side effects from X-rays
- Stroke
How do I prepare for cardiac catheterization?
- You will be told what you can eat and drink 24 hours before the test.
- You usually will be asked not to eat or drink anything for six to eight hours before the procedure.
- Tell your health care team if you think you might be pregnant.
- Tell your health care team about any medications you take, including Viagra or other medications for erectile dysfunction.
- Tell your health care team if you are allergic to anything, especially:
- Iodine
- Shellfish
- Latex or rubber products
- X-ray dye
- Medications
- Have someone drive you home after your procedure.
- If you have a hearing aid, you can wear it during your procedure.
- If you wear glasses, bring them to your appointment.
What happens during cardiac catheterization?
A doctor with special training performs the procedure with a team of nurses and technicians. The procedure is done in a cath lab at a hospital or medical clinic.
- Before the procedure, a nurse will put an IV line into a vein in your arm so you can get medication to help you relax. You will be awake and able to follow instructions during the procedure.
- The nurse will clean and shave the area where the doctor will be working. This could be in the upper thigh, arm or neck or under the collarbone.
- A local anesthetic is usually given to numb the puncture site.
- The doctor will make a needle puncture through your skin and into a large blood vessel. A small straw-sized tube will be placed into the vessel. The doctor will gently guide a catheter into your vessel through the sheath. A video screen will show the position of the catheter as it is threaded through the blood vessels and to the heart. You may feel some pressure at the procedure site, but you shouldn’t feel any pain.
- The doctor may use the catheter plus other instruments to:
- Inject a dye to look at blood flow in the heart
- Look at the inside of blood vessels
- Take tissue samples from the heart to study
- Clear a blocked artery
- Open a partially blocked heart valve
- When the procedure is complete, the doctor will remove the catheters and the sheath. Your nurse will put pressure on the site to prevent bleeding. Sometimes, a special closure device is used.
What happens after cardiac catheterization?
You will go to a recovery room for a few hours. During this time, you must lie flat.
- Pressure will be applied to the puncture site to stop any bleeding.
- You will be asked to keep flat the site where the catheter was placed. You will not be able to get out of bed.
- Your heartbeat and blood pressure will be checked during your recovery.
- Report any swelling, pain or bleeding at the puncture site, or if you have chest pain.
- If you had an additional procedure during the cardiac cath, you may have to spend the night in the hospital.
- Before you leave the hospital, you will get written instructions about what to do at home.
What happens after I get home?
Be sure to follow all the instructions provided by your health care team. It is important to take your medications as directed and to make follow-up appointments before leaving the hospital. Most people can return to their normal activities the day after the procedure, depending on whether any other procedures were done during the cardiac cath.
A small bruise at the puncture site is normal. If the site starts to bleed, lie flat and press firmly on it for a few minutes. Then, recheck to see if the bleeding has stopped.
Call your health care professional if:
- The puncture site becomes numb or tingles, or your foot feels cold or turns blue.
- The area around the puncture site looks more bruised.
- The puncture site swells or fluids drain from it.
- Bleeding from the access site can’t be stopped with firm pressure.
- You are coughing up blood or yellow or green mucus.
- You have problems taking any of your heart medications.
- You have:
- Chest pain or shortness of breath
- Dizziness
- Fever
- Irregular, very slow or fast heartbeat
Call 911 if:
- The puncture site swells up very fast.
- Bleeding from the puncture site does not slow down when you press on it firmly.