Myocarditis
What is myocarditis?
Myocarditis is a serious yet rare condition where inflammation develops in the myocardium, the middle muscular layer of the heart wall.
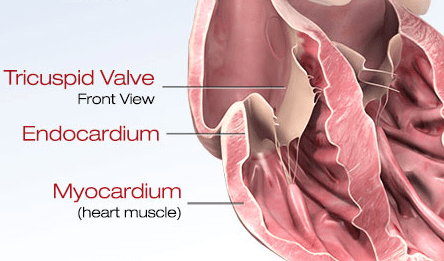
Myocarditis can weaken the heart and its electrical system. As a result, the heart’s ability to pump blood is reduced.
The condition may be acute and resolve quickly , or it may be subacute or chronic, lasting up to three months. In severe cases, myocarditis may lead to heart failure or death.
Commonly a viral infection (such as the flu), bacterial infection (such as staph or strep) or fungal infection (such as candidiasis) can lead to myocarditis. Medications, autoimmune disorders and toxic substances can also cause it.
What are the symptoms of myocarditis?
People with myocarditis don’t always have symptoms. Others have mild or severe signs, such as:
- Fatigue or exercise intolerance
- Shortness of breath
- Fever
- Chest pain
- Hard, rapid or irregular heartbeat
- Lightheadedness or fainting
- Flu-like symptoms including headache, body ache, joint pain or sore throat
Some cases of myocarditis can feel like a heart attack. Seek emergency medical help right away for unexplained chest pain or shortness of breath.
How is myocarditis diagnosed and treated?
A health care professional is needed to diagnose myocarditis. They will do a physical exam and get the patient’s medical and family history. In addition, other procedures are used to diagnose the condition, including:
- Blood tests
- Cardiac MRI (CMR)
- Chest X-ray
- EKG/ECG (electrocardiogram)
- Echocardiography, also called ultrasound
- Cardiac catheterization with coronary angiography and biopsy
Myocarditis treatment targets symptoms and the underlying cause if it is known. Those with mild myocarditis may need only rest and medication. People with severe cases may need lifelong medication, implanted devices or other surgeries.
Staying healthy
Proper heart function can be supported by lifestyle changes. Some of these include reducing sodium intake, avoiding alcohol and quitting smoking. People with myocarditis are often advised to avoid competitive sports while active inflammation is present.
Myocarditis and COVID-19
Health organizations such as the Centers for Disease Control and Prevention (CDC) continue to monitor whether myocarditis is linked to COVID-19. The CDC stated that myocarditis after the COVID-19 vaccine is rare. Myocarditis was reported at a higher rate than expected among some people who received the Pfizer or Moderna vaccines, according to one study. Most of the suspected myocarditis cases in that study developed after the second dose. Another study found that 20% of people hospitalized due to COVID-19 infection developed new onset myocarditis, which greatly increased mortality and ventilation rates.






