Why Atrial Fibrillation Matters
Quick Facts
- Atrial fibrillation (AFib) can increase your risk for stroke and related heart problems.
- There are treatments and medications for AFib. But sometimes it never goes away.
Video: Identify your potential AFib risks
What are the effects of atrial fibrillation?
Atrial fibrillation, also called AFib or AF, can feel weird and scary. But an “AFib attack” usually doesn’t have harmful outcomes by itself. One of the real dangers is the increased risk for stroke. Even when you don't feel symptoms, AFib can still increase your risk for stroke and related heart problems.
What causes AFib?
Sometimes, the cause of AFib is unknown. Other times, it is the result of damage to the heart's electrical system from other conditions, including:
- Long-term, uncontrolled high blood pressure
- Coronary artery disease
- Complications after surgery. AFib has been reported as the most common arrhythmia after some heart surgeries.
Can AFib lead to other problems?
AFib can lead to other medical problems, including:
- Stroke
- Heart failure
- Other heart rhythm or rate problems
- Poor blood flow to the body
Learn about the connection between atrial fibrillation, high blood pressure and stroke.
How does AFib lead to stroke?
- The heartbeat seems to quiver in an erratic way. The upper chambers of the heart (the atria) contract irregularly.
- The contraction fails. Imagine wringing out a sponge. Without a good squeeze, water will still be left in the sponge. In the same way, when the heart contracts too fast or unevenly, it doesn’t completely squeeze the blood from the atria into the next chamber.
- Blood pools in the atria. Blood not pumped out of the atria can remain and may pool there.
- Risks of clotting increase. When blood can pool, it can form clots.
- Clots can travel and cause blockages. If a blood clot forms in the atria, it can be pumped out of the heart to the brain. This can block the blood supply to an artery in the brain and cause a stroke. This type of stroke is called an embolic stroke, which is a type of ischemic stroke.
How does AFib lead to heart failure?
Heart failure means the heart isn’t pumping enough blood to meet the body’s needs. AFib can lead to heart failure in part because the heart is beating so fast or unevenly that it never properly fills up with blood to pump out to the body.
When the heart doesn’t efficiently pump the blood forward, symptoms develop because:
- Blood can “back up" in the pulmonary veins, the vessels that return oxygen-rich blood from the lungs to the heart. This can cause fluid to back up into the lungs.
- When AFib causes heart failure, fluid in the lungs can cause fatigue and shortness of breath. Oxygen-rich blood may not be delivered to the body and brain. This can cause physical and mental fatigue and weakness. Fluid also can build up in the feet, ankles and legs, causing weight gain.
How does AFib lead to more heart rhythm problems?
Basic answer: The heart’s electrical system stops working properly and fails to keep the heart chambers in rhythm.
Thorough answer: Every heartbeat is controlled by the heart’s electrical system. To understand why AFib is a problem, it's helpful to understand the normal patterns of the heart’s electrical system.
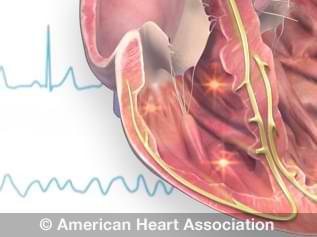
View an animation of a normal heartbeat.
In a normal heartbeat:
- The current travels from top to bottom. The heartbeat starts at the top of the heart like an electrical wave. The signal moves from the top of the heart to the bottom. This tells the tissue to contract.
- The sinoatrial (SA) node starts the contraction at the top of the heart. The right atrium (one of the two types of chambers of the heart) houses a group of cells called the sinoatrial node. In a normal heartbeat, the node fires between 60 to 100 heartbeats per minute. The electrical wave moves through the atria to the “gatekeeper node.”
- The atrioventricular (AV) node controls the timing for the lower portion of the heart. This node is a gatekeeper for all the electrical pulses going through the atria (top sections) to the ventricles (bottom sections). The pulses are delayed at the AV node before they are allowed to move into the ventricles. This delay gives the ventricles extra time to fill with blood before contracting.
- The ventricles contract and pump blood to the lungs and the body.
Electrical problems in AFib:
- The SA node may not start the contraction. Instead, the contraction might start randomly in other areas of the atria or pulmonary veins.
- The electrical current doesn’t flow in an organized top-to-bottom pattern. Instead, contractions are rapid and disorganized.
- The AV node often can’t regulate the chaotic current. It does its best to protect the ventricle from extra pulses , but it can’t stop all of them. As a result, the ventricle beats more often than it should. This leads to breathlessness and fatigue.
- When the beat is off, the blood supply can be unpredictable. Even though the ventricles may be beating faster than normal, they aren't beating as fast as the atria. So, the atria and ventricles no longer beat in a coordinated way. This creates a fast and irregular heart rhythm. In AFib, the ventricles may beat 80 to 180 times a minute, in contrast to the normal rate of 60 to 100 beats a minute.
The amount of blood pumped out of the ventricles to the body is based on the randomness of the atrial beats.
The body may get rapid, small amounts of blood and occasional larger amounts of blood. The amount will depend on how much blood has flowed from the atria to the ventricles with each beat.
Can AFib simply go away?
Overall, most risks, symptoms and outcomes of AFib are related to:
- How fast the heart is beating
- How often abnormal rhythms happen
AFib may be brief, with symptoms that come and go. An AFib episode may resolve on its own, or it may be persistent and need treatment. Sometimes AFib is permanent. Medications or other treatments can’t restore a normal heart rhythm.
It’s important to work with your health care professional to decide on your treatment needs and understand your options. It's also important to maintain a heart-healthy lifestyle to reduce your overall risks as much as possible.






