Heart Conduction Disorders
Rhythm versus conduction
Your heart rhythm is the way your heart beats. Conduction is how electrical impulses travel through your heart, which causes it to beat. Some conduction disorders can cause arrhythmias, or irregular heartbeats.
Three common conduction disorders are:
Bundle branch block
Normally, electrical impulses travel down the right and left bundle branches of the ventricles at the same speed. This allows both ventricles to contract at the same time.
But when there’s a “block” in one of the branches, electrical signals must take a different path through the ventricle. This detour means that one ventricle contracts a fraction of a second slower than the other, causing an abnormal heartbeat.
Symptoms and diagnosis
A person with bundle branch block may feel no symptoms, especially in the absence of any other problems.
In such cases, bundle branch block is usually first identified by testing for some other reason, such as a routine physical. An electrocardiogram (EKG or ECG) can detect bundle branch block.
Treatment
Often, no treatment is required for bundle branch block. But there are cases where treatment may be needed.
It’s still important to have regular checkups. Your health care professional will want to monitor your condition to make sure that no other changes occur.
Heart block
Heart block is a delay in the electrical signals that progress from the heart’s upper chambers (atria) to its lower chambers (ventricles). When those signals don’t transmit properly, the heart beats irregularly.
There are many degrees of heart block.
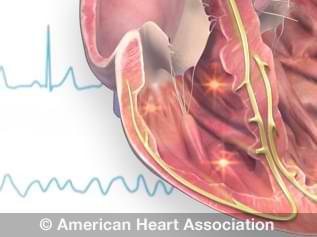
Watch an animation of heart block.
First-degree heart block
First-degree heart block occurs when the electrical impulse moves through the heart’s AV node slower than normal. This usually results in a slower heart rate. First-degree heart block rarely causes symptoms and may not need treatment.
Some medications can cause first-degree heart block as a side effect:
- Digitalis: This medication is used to slow down the heart rate. If it’s taken in high dosages or for a long period, digitalis can cause first-degree heart block.
- Beta blockers: These drugs inhibit the part of the nervous system that speeds up the heart. This can have the side effect of delaying electrical conduction within the heart, which can cause first-degree heart block.
- Calcium channel blockers: Among other effects, calcium channel blockers can slow down the conduction within the heart’s AV node, resulting in first-degree heart block.
If you have first-degree heart block, it’s important to check in regularly with your health care professional to monitor the condition. Between medical appointments, you should take your pulse regularly and watch out for slower-than-normal heart rates.
Second-degree heart block
Second-degree heart block occurs when only some electrical signals from the heart’s upper chambers reach the lower chambers. This can cause the heart to miss beats and beat slowly and irregularly.
Some symptoms of second- and third- degree heart block include:
- Chest pain
- Fainting or feeling faint
- Dizziness
- Heart palpitations
- Shortness of breath
- Labored breathing during sleep
- Nausea
- Fatigue
Second-degree heart block can be classified in two ways:
- Mobitz Type 1: Mobitz Type 1 may not cause noticeable symptoms. But it can be a forerunner for the more serious Mobitz Type 2. For this reason, Mobitz Type 1 should be monitored carefully by your health care professional. Daily pulse checks on your own may also be advised.
- Mobitz Type 2: In this type of second-degree heart block, the heart doesn’t beat effectively. It impacts the heart’s ability to pump blood throughout the body. Often, a pacemaker is needed to ensure that the heart will continue to beat regularly and efficiently.
Third-degree heart block
In third-degree, or complete, heart block, electrical signals can’t pass from the heart’s upper chambers to its lower chambers. Without electrical impulses from the sinus node, the ventricles will still contract and pump blood, but at a slower rate than usual.
With third-degree heart block, the heart does not contract properly, and it can’t pump blood out to the body effectively.
Third-degree heart block may be caused by:
- Certain medications
- A heart attack that damages the heart’s electrical conduction system
- Heart surgery
- Heart diseases, such as heart valve disease
- Some infections, such as Lyme disease
People with third-degree heart block require immediate medical attention. Their irregular and unreliable heartbeats heighten the risk of cardiac arrest.
A temporary or permanent pacemaker is used to treat third-degree heart block. If medications are causing the heart block, changing medications may fix the problem.
Long QT Syndrome
Long QT Syndrome, also called LQTS, is a disorder of the heart’s electrical system, like other arrhythmias. LQTS can cause abnormal heart rhythms in response to exercise or stress.
In LQTS, the heart's lower chambers take too long to contract and release.
The name comes from letters associated with the waveform created by the heart’s electrical signals. The interval between the letters Q and T defines the action of the ventricles.
An occasional prolonged QT interval can be caused by everyday events, such as:
- Being startled by a noise
- Physical activity or exercise
- Intense emotion (such as fright, anger or pain)
In these instances, the heartbeat usually regains its normal rhythm quickly. However, medication may be helpful in controlling the condition.
Both hereditary and acquired
LQTS can be hereditary, appearing in otherwise healthy people. (Although this happens infrequently.) When this occurs, it usually affects children or young adults.
Other people acquire LQTS, sometimes as a side effect of medications. It’s also possible for someone to have both the hereditary and acquired forms of LQTS.
Medications that can cause LQTS
Many types of medications can cause LQTS, including:
- Antihistamines and decongestants
- Diuretics (such as potassium or sodium)
- Certain antibiotics
- Antiarrhythmia medications (meds that regulate heartbeat)
- Antidepressant and antipsychotic medications
- Cholesterol-lowering medications
Symptoms of LQTS
People with LQTS may not have any symptoms. Those who do may experience:
- Fainting (syncope)
- Fluttering in the chest
- Abnormal heart rate or rhythm
- Gasping while sleeping
- Seizures
Diagnosing LQTS
If LQTS is suspected, your health care professional will want to ask questions about your medical history, as well as your family’s.
Unexplained fainting episodes or a family history of heart-related death may warrant electrocardiogram (ECG) testing for you and your closest relatives. Your health care professional may also recommend an exercise stress test.
Consequences of LQTS
Some arrhythmias related to LQTS can be fatal and can cause sudden cardiac arrest. Deafness also may occur with one type of inherited LQTS.
If you have been diagnosed with LQTS, talk with your health care professional about what types and amounts of physical activity are safe for you. In some cases, exercise, especially swimming, can bring about fatal arrhythmias in those with LQTS. You should ask your cardiologist what activities you should avoid.
Treatment for LQTS
Treatment options for LQTS include:
- Medications, such as beta blockers
- Surgical procedures
- Implantable cardioverter defibrillator (ICD) or pacemaker






